Human-AI Collaboration in Healthcare: A Look at the Next Decade
The Dawn of a New Era in Medicine
Artificial intelligence (AI) is set to revolutionize healthcare, transforming medical practices and patient care in ways once considered unimaginable[6]. The integration of AI promises to mitigate shortages of qualified healthcare workers, assist overworked professionals, and improve the overall quality of care[1]. This technological shift is not about replacing human expertise but augmenting it; AI is perceived as a supplement, not a replacement for the skill of a human surgeon[9]. AI systems can provide insights and recommendations that complement a physician's knowledge, empowering them to critically assess recommendations and ensure they align with clinical evidence and patient needs[5]. As this human-AI collaboration evolves, it stands to create a future optimized for the highest quality patient care[10].
Collaborative Diagnostics and Personalized Treatment
One of the most profound applications of AI in healthcare is in diagnostics, where machine learning algorithms interpret medical data such as imaging, lab results, and patient histories more efficiently and accurately than traditional methods[6]. AI is particularly useful for identifying subtle patterns in large datasets that may be imperceptible to humans[10]. For instance, deep learning algorithms have successfully identified abnormalities like calvarial fractures and intracranial hemorrhage from CT scans, showcasing the potential for automating triage in emergency care[9]. Beyond diagnostics, AI is a powerful tool in precision medicine, enabling the development of individualized treatment plans tailored to each patient’s specific needs by integrating data from genetic profiles, lifestyle habits, and clinical history[6][11]. The future points towards predictive care, where AI will assist providers in disease prediction. Technological advances aim to help radiologists predict if a patient will develop lung or breast cancer sooner and determine how well a patient might respond to specific treatments[4].
AI-Powered Surgical Assistance
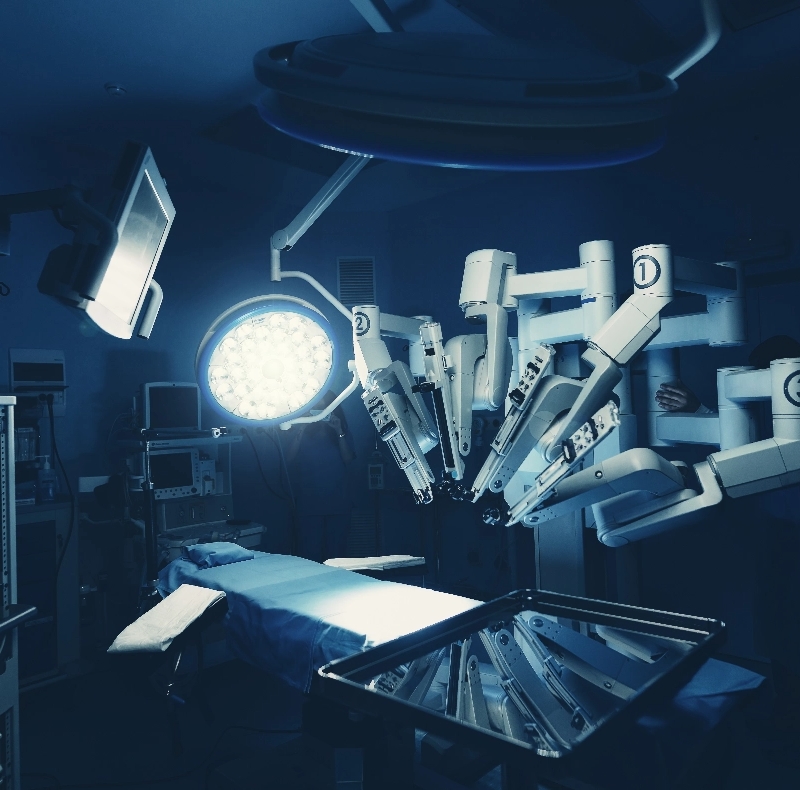
In the surgical field, AI is driving significant changes for both doctors and patients[9]. During preoperative planning, AI enables precise surgical plans, which minimizes errors, shortens surgical duration, and reduces postoperative complications[11]. Intraoperatively, AI-driven surgical robots, such as the da Vinci Surgical System, offer enhanced dexterity, improved visualization, and reduced tremors compared to traditional methods[3][11]. These robots assist surgeons by automating repetitive tasks like suturing and tissue dissection, which enhances consistency and reduces surgeon workload[3]. Systems like the Smart Tissue Autonomous Robot (STAR) have demonstrated the ability to match or even surpass human surgeons in autonomous bowel anastomosis in animal models[10]. The evolution of surgical robotics is framed by levels of autonomy, from Level 0, where surgeons directly control the robot, to the aspirational Level 5, where a robot would perform surgery without human intervention[3]. Currently, AI also provides computer-assisted intraoperative guidance, with real-time analysis of laparoscopic video offering a form of clinical decision support[9][10].
Revolutionizing Patient Engagement

AI is transforming the interaction between healthcare providers and patients, moving beyond standard, one-size-fits-all adherence programs to sophisticated, individualized support[8][12]. AI-powered tools like chatbots and virtual assistants provide patients with 24/7 support, answering queries and scheduling appointments[8]. This constant connectivity helps patients feel supported throughout their care journey[8]. Predictive analytics can identify patients at risk of missing appointments or not adhering to treatment plans, allowing providers to intervene proactively[8][7]. Furthermore, AI streamlines administrative workflows by automating tasks like managing digital intake forms and patient scheduling, which reduces waste and lowers costs[4]. Innovative applications are also emerging, such as enhanced virtual waiting rooms that engage patients with informational media and the ability to capture vital signs remotely using a device's web camera[4]. Ultimately, when patients have an easy, efficient, and rewarding experience, their engagement increases, leading to better health outcomes and higher retention in clinical trials[4][7].
Essential Safeguards for Responsible Implementation

The integration of AI into healthcare brings a host of challenges related to ethical and legal considerations[6]. A primary concern is accountability. AI-based tools challenge standard clinical practices of assigning blame, as clinicians have weaker control over and less understanding of how AI systems reach decisions[2]. This raises complex questions about who is liable for errors: the provider, the AI developer, or the hospital[6]. There is a need to include AI developers and systems safety engineers in assessments of moral accountability for patient harm[2]. Another significant issue is algorithmic bias. If AI systems are trained on data that lacks diversity or reflects societal biases, they can generate unfair outcomes that perpetuate existing healthcare disparities[5][7]. For example, one healthcare algorithm systematically disadvantaged Black patients because it was trained on healthcare spending rather than patient needs[6]. To mitigate this, AI should be trained on diverse datasets, and systems must be continuously monitored and refined[5]. Data privacy is also paramount, as AI systems are treasure troves of valuable data, making them prime targets for cyberattacks[5]. Robust security protocols and compliance with regulations like HIPAA and GDPR are essential to safeguard patient information[5][6]. Finally, the 'black box' nature of some AI algorithms, where their decision-making process is opaque, underscores the need for human oversight[10]. AI should serve as a tool to support, not replace, human judgment, and the final decision-making power must remain in the hands of human doctors[5][11].
The Path Forward: An Integrated Future
The future of AI in healthcare lies in a human-machine collaboration model that drives progress in the medical field[11]. For this collaboration to succeed, robust ethical and legal frameworks are needed to guide its adoption[6]. Given the rapid evolution of AI, regulations must be adaptive, with periodic reviews and updates to address emerging risks and opportunities[6]. International cooperation is also critical to harmonize regulatory processes and establish global standards for AI data privacy, transparency, and accountability[6]. Surgeons and other clinicians are uniquely positioned to help drive these innovations by partnering with data scientists to capture novel data and generate meaningful interpretations[10]. While many challenges remain, such as investigating biases and addressing adoption issues, the continued development of collaborative AI holds the potential to create a more efficient, accessible, and patient-centered healthcare system[1][10].
Get more accurate answers with Super Pandi, upload files, personalized discovery feed, save searches and contribute to the PandiPedia.
Let's look at alternatives:
- Modify the query.
- Start a new thread.
- Remove sources (if manually added).

.png)